A cancer diagnosis is often difficult to take in and everyone will have a different reaction. Feelings of shock, anger, sadness, fear and helplessness may occur. Making sense of what happens next can be difficult.
Everyone reacts to a diagnosis of cancer differently. It is often difficult to take in the diagnosis immediately. It is normal to ask ‘why me?’ or to feel sad, angry, helpless or worried about your future. Talk to your doctor about what your diagnosis means for you. The outlook for many cancers is improving constantly.
Sharing your diagnosis isn’t easy. You may feel uncomfortable talking about it. You may be unsure how you will react when you tell your family and friends and how they will respond. Having other people know will help you and your family share your anxiety and fears. You don’t have to face cancer alone.
CANCER, WHAT IS IT?
Cancer is a disease of the cells. Cells are the body’s basic building blocks – they make up tissues and organs. The body constantly makes new cells to help us grow, replace worn-out tissue and heal injuries. Normally, cells multiply and die in an orderly way, so that each new cell replaces one lost. Sometimes, however, cells become abnormal and keep growing. These abnormal cells may turn into cancer.
In solid cancers, such as cervical or bowel cancer, the abnormal cells form a mass or lump called a tumor. In some cancers, such as leukemia, abnormal cells build up in the blood.
RADIATION THERAPY
Radio Therapy (RT) kills tumor cells with high-energy x-rays (photons), gamma rays, or protons. It usually follows surgery. Radiation kills tumor cells that may remain in the area, following surgery.
Sometimes, people who can’t have surgery have radiotherapy instead. It may also be given in combination with chemotherapy.
Overall, radiotherapy is required by 50% of all cancer patients. It is one of the most effective treatments for cancer.
It can be used in three main ways:
RADIATION THERAPY
– To achieve remission or cure: radiation therapy may be given as the main treatment to cause cancer to reduce (remission) or disappear (curative or definitive radiation therapy).
– To help other treatments: radiation therapy is often used before other treatments to shrink the tumor or after other treatments to kill any remaining cancer cells.
– To relieve symptoms: radiation therapy can help to relieve pain and other symptoms by making cancer smaller or stopping it from spreading. This is known as palliative treatment.
Treatment is carefully planned by the radiotherapy team around any patient in order to hit selectively malignant tissue, identifying with precision the target tumor, saving the surrounding healthy tissues, preserving the organs and their functions, and reducing the duration of the treatment.
There are two main ways of giving radiation therapy: from outside the body or inside the body. You may have one or both types of radiation therapy, depending on the cancer type and other factors.
– External beam radiation therapy (EBRT) Radiation beams from a large machine called a linear accelerator are precisely aimed at the area of the body where the cancer is located. The process is similar to having an x-ray.
You will lie on a treatment table underneath a machine that moves around your body. You won’t see or feel the radiation, although the machine can make noise as it moves.
– Internal beam radiation therapy (IBRT): a radiation source is placed inside the body or, more rarely, injected into a vein or swallowed. The most common form of internal radiation therapy is brachytherapy, where radiation sources are placed inside the body next to or inside cancer.
Conditions Treated
– Arteriovenous malformations: an abnormal set of connections between arteries and veins usually occurring in the brain and spine, causing neurologic symptoms or bleeding.
– Bone cancer: an abnormal growth of cells within a bone that may be cancerous or benign.
Acoustic neuroma An abnormal growth of tissue (tumor) in the brain that may be cancerous or non-cancerous.
– Breast cancer: a disease in which malignant cancer cells form in the tissues of the breast.
– Chondrosarcoma: a malignant type of bone cancer that primarily affects the cartilage cells of the femur (thighbone), arm, pelvis, knee, and spine. Although less frequent, other areas (such as the ribs) may be affected.
– Chordoma: a rare type of slow-growing cancerous tumor that can occur anywhere along the spine, from the base
of the skull to the tailbone.
– Colorectal cancer: a disease that is indicated by malignant cells in the colon or rectum.
– Esophageal cancer: a disease in which cancerous cells form in the tissues of the esophagus.
– Ewing’s sarcoma: a type of cancer that occurs primarily in the bone or soft tissue, most often found in the extremities and can involve muscle and the soft tissues around the tumor site as well as spread to other areas of the body.
– Head and neck cancers: benign and malignant tumors that originate in the head and neck region, including sarcomas and nerve or lymph node conditions.
– Leukemia cancer: of the blood that develops in the bone marrow, which produces the three major blood cells: white blood cells, red blood cells, and platelets.
– Liver cancer: a type of cancer that starts in the cells of the liver. Viral hepatitis and liver damage from alcohol or fatty liver are risk factors for liver cancer.
– Lung cancer: cancer that usually starts in the lining of the lungs, but can also begin in other areas of the respiratory system.
– Lymphoma cancer: starts in cells called lymphocytes, which are part of the body’s immune system.
– Metastatic brain cancer: An abnormal growth of tissue (tumor) in the brain that travels from another part of the
body to the brain (metastasize).
– Meningioma: a type of tumor that grows from the protective membranes, called meninges, which surround the
brain and spinal cord, and is often benign and slow-growing.
– Non-Hodgkin’s lymphoma: a type of cancer of the lymphatic system that can begin in almost any part of the
body, causing cells to abnormally reproduce and tumors to eventually grow.
– Osteosarcoma: a type of bone cancer, most often occurring in children, adolescents, and young adults, that develops
in the osteoblast cells that form the outer covering of bone.
– Pancreatic cancer: cancers that begin in the pancreas.
– Prostate cancer: a type of cancer that occurs when cells grow abnormally in the prostate gland and form tumors.
– Soft tissue sarcomas: rare cancer in one of the soft tissues. There are many different kinds of soft tissue sarcoma.
In general, soft tissue sarcomas are rare.
– Paranasal sinus cancer: a tumor that forms on the spinal cord or in the area around it. Even if benign, the tumor
may cause pain, weakness, numbness, or tingling from pushing on the spinal cord or nerves.
– Trigeminal neuralgia: a nerve disorder that causes a stabbing or electric-shock-like pain in parts of the face.
Learn more about our equipment
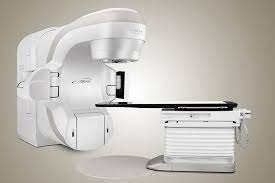
TRUEBEAM VARIAN
TrueBeam system brings leading-edge cancer care to communities by positioning clinics at the forefront of the fight against cancer. Designed from the ground up to treat moving targets with advanced speed and accuracy, the TrueBeam platform is a fully-integrated system for image-guided radiotherapy and radiosurgery. TrueBeam treats cancer anywhere in the body where radiation treatment is indicated, including lung, breast, prostate, and head and neck.
The number of physicians adopting advanced treatments like Stereotactic Body Radiation Therapy (SBRT) is rising. Technologies such as motion management, integrated imaging, and high dose rates are some of the tools that are required for the delivery of advanced treatments like stereotactic body radiation therapy.
The carefully guided, automated workflow on the TrueBeam system uses intuitive visual cues to enhance safety and reduce operation times so patient throughout can be optimized. Streamlined imaging and patient positioning tools enable more flexibility to treat clinical cases throughout the body.
Having the power to not only treat quickly, but to deliver high, accurate dose rates are hallmarks of the TrueBeam system. Clinics worldwide have already adopted the TrueBeam system to help advance the way cancer is treated.
Simple treatments that once took 10 to 30 minutes can now be completed in less than two minutes.
As well as allowing for a more comfortable experience for the patient with less time on the treatment couch, faster delivery also allows for reduced chances of tumor motion during treatment, which helps protect nearby healthy tissue and critical organs.
The precision of the TrueBeam system is measured in increments of less than a millimeter. This accuracy is made possible by the system’s sophisticated architecture, which synchronizes imaging, patient positioning, motion management, beam shaping and dose delivery, performing accuracy checks every ten milliseconds throughout the entire treatment.
Imagine a tumor no larger than a few millimeters wide about the size of a pencil tip. That’s where TrueBeam Radiotherapy comes into play.


No comment